“Doctor Google” goodbye: towards certified and validated self-diagnosis systems
7 May 2019 | Written by Thomas Ducato
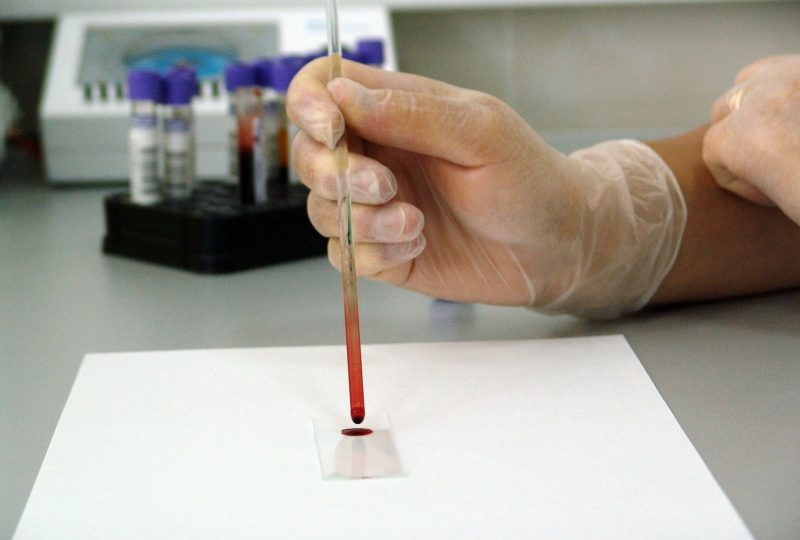
We interviewed Marco Vismara, medical geneticist, and Antonio Valentini, biologist, of lightScience, a startup that deals with blood analysis through the use of IoT medical systems
The combination of technology and medicine is well-established and is profoundly changing the world of health. A revolution that, according to the latest report StartUp Health Insights has even led to a turning point with the overcoming of the concept of Digital Health: speaking of “digital health” today, in fact, seems almost reductive if we consider the number of areas involved and the market that revolves around these solutions technology. The most correct term, therefore, seems to be Health Innovation: a healthy sector (from every point of view), in which researchers and professionals, but also entrepreneurs and investors, believe.
Self-diagnosis and access to care. Among the areas in which greater energy and resources are being concentrated there is that of self-diagnosis. Thanks to sensors, nanotechnologies, and IoT systems, the Internet of Things, users have access to increasingly reliable systems to monitor their health, at least partially avoiding the use of “Doctor Google”, with the consequent risk of running into fake news or misdiagnosis.
These devices can also represent a turning point to guarantee access to care for people living in remote areas of the planet, in places without adequate health facilities or patients with mobility problems.
lightScience AI. In this context is born lightScience.AI, a startup that is planning a portable blood analysis system, to be launched on the market of self-diagnostic devices.
We interviewed the founders of the project Marco Vismara, a medical geneticist, and Antonio Valentini, a biologist, to find out more about this innovative startup in the HealthCare sector.
What does lightScience do and how was it born?
A: In a nutshell, lightScience deals with blood analysis through the use of IoT medical systems. The project was born from the need to find a way to reach those who need analysis independently of geographical barriers, reducing displacement of patients who have mobility problems, or reaching people who live in remote areas without the need to lean on a hospital. With this system, it is the analysis that goes from the patient, with a view to decentralization.
When did you start thinking about this technology?
M: The reasoning started from phenylketonuria, the most common of the rare diseases I have dealt with during my career. In Italy, there are only 12 laboratories able to perform the control tests, which are performed very often, up to twice a week. It is easy to imagine the impact this has on the lives of patients with this condition.
Solutions are already in use, for example by mail, but they are not immediate at all. When the first low-cost spectroscopic sensor entered the market, we were lucky enough to buy it before it was even officially released. Everything was born from here.
Then, after the preliminary results obtained with phenylketonuria, we began to think about the impacts of this innovation also in other parts of the world, starting from Africa where we had contacts: in countries where conditions are different and distances to go for having access to treatments are extremely large, this type of technology could also be important for more common pathologies, such as for infectious diseases.
So in developing the idea, did you start from a concrete need?
M: We can say that it was a “bottom-up” process, in the sense that we started from a need that we touched with our hands during a direct experience. In particular, I worked in one of the 12 Italian centers that deal with the control test for phenylketonuria, so in my daily work, I have repeatedly touched the need to decentralize the process. Antonio is a biologist and works in analysis laboratories, so we both know the impacts that this innovation can bring to people’s lives.
Which one?
A: The impacts, if we could spread this system on a large scale, will be enormous and will not only affect the lives of patients and their families, which can save a lot of time for work or personal matters.
They will also be of an environmental nature because compared to the classic analysis laboratory waste is reduced, the production of special waste, reagents used for classical analyzes. Even if in a secondary way there would be a reduction of CO2 emissions, linked to the elimination of travel to reach the laboratories.
On the other hand, the spread of our and all other self-diagnostic devices will lead to an increase in data availability: this will require the creation and use of new tools and infrastructures. This, however, holds for the whole sphere of telemedicine, which will have a potentially immense impact.
And from an ethical point of view?
M: The national Italian bioethics consultation expressed itself in 2016 precisely on big data and communication, especially in the health sector. It was important for us to hear that there was an interest in the scientific community for these issues. We committed ourselves immediately, not only to respect the law in the strict sense but also to develop all our products taking into account bioethical guidelines national and foreign that we believe are fundamental for the future development of the sector.
Also because we are dealing with very sensitive data, which is not always treated as it should be. Privacy and civil rights, as principle of transparency and open and declared governance on data management, are aspects to which we care a lot and we want to be a proactive part in the construction of the new ecosystem.
How do you imagine the role of the doctor in this context?
A: Compared to other self-diagnostic products on the market, ours is slightly different: the patient will obtain results and analyzes approved and validated by health personnel. The difference is that the data to be analyzed will not pass from one laboratory to another but in a cloud. The professional will not be physically present to look at the data on a sheet of paper, but will be in front of a monitor: his role and his task, however, will not change. We could, therefore, define our system more telediagnostic than self-diagnostic.
So, in detail, how does the system work?
M: The idea is to add an abstraction layer to blood tests, with the early digitization of the sample. It may seem a complex concept but in reality it is quite simple: we want the person to be able to take the blood autonomously using simplified techniques, such as the puncture of the finger already widespread for the measurement of insulin in diabetics. From this sample, digitization takes place immediately, thanks to IoT sensors. Once the data path is digitized, in reality it remains the same as the classic analysis laboratory: the same supply chain is maintained and, therefore, the same quality, but everything moves to a cloud. The philosophy behind it all is that innovation can also be made starting from “old” concepts and mechanisms, put together in a new way. But it is important to start from solid foundations rather than ride the technological hype.
What technologies do you use?
M: The ones we use are all well established technologies: spectrometry, chemiometry, supports to deposit the sample have been used since the 60s, cloud. It is true that the spectroscopes we use are super miniaturized, that modern clouds have unimaginable computational power until recently, but these are technologies that give us ample security.
We have only mentioned the issue of privacy. How will the data be managed?
A: Obviously we will collect data and this is particularly sensitive information: in addition to the personal data, we have access to biological samples of the person. It is extremely important, therefore, that there is seriousness and transparency in the processing of data, it is one of the great new challenges of technological development.
Our background has led us to address this issue with the utmost care and seriousness: we strongly believe in the professional secrecy and alliance that must be created between the patient and the care provider. The patient is and must be the master of his data, we are custodians.
Where are you with development today?
M: We did preliminary experiments and feasibility studies, achieving positive results, and obtained the first patent, which was granted to us a few months ago.
Ours is a modular model: we started with phenylketonuria but we have the idea of starting new modules, each with its own supply chain.
In the future, the project is to build around the data analysis a complete platform, which can be gradually implemented. For example, in addition to the analysis, we will also be able to offer real medical consultations in telemedicine: when there is a wrong value we would like to offer the opportunity to have a consultation with a specialist, thus overcoming the informal consultation, via email or even WhatsApp, which is being developed.
But first, we must certify our project and have all the necessary accreditations. It will be a long but necessary process.
So when do you think it can be available?
A: We are counting on marketing the system for the first analyzes in 2021: we would like to immediately present an official and tested version, in terms of health we are not joking and a beta version is not admissible.
What is the innovation situation in the health care sector? What technologies will most change this sector in the near future?
A: The real challenge will be to standardize the data, find a format that makes digital medical records valid and legible anywhere.
M: I believe that normative work will be needed soon because the diffusion of these technologies will require an update from this point of view. There are many technologies in the field and I truly believe that they will change not only the health sector but, more generally, the world in which we live.